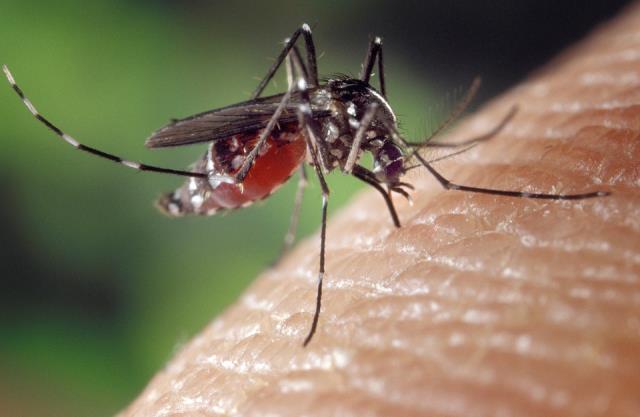
Mosquito-transmitted virus on the rise
Digital Edition
Subscribe
Get an all ACCESS PASS to the News and your Digital Edition with an online subscription
North Burnett’s Anzac Day guide
Communities throughout the North Burnett will commemorate the immortal landing at Gallipoli on Saturday.
The North Burnett's Anzac Day events this year take place in...







